The following is a guest blog post by Mary Sirois and Heather Haugen PhD from Atos Digital Health Solutions.


The topics of Population Health and Value Based Care continue to swirl through nearly every healthcare conversation. Leaders across the healthcare provider and payer industries are looking for strategies to reduce costs and improve quality in hopes of improving the bottom line and increasing the viability of the organization within the community; and every vendor has a solution. We recently formed an expert panel to study and better understand the current state of work being done across healthcare provider organizations. We explored the topics of leadership strategy and commitment, data aggregation, data analytics, and consumer engagement. Our conversations reinforced the importance of developing a research-based approach to help healthcare leaders navigate the breadth and depth of this critical initiative: value based care. Our findings continue to drive our work in defining solutions that meet healthcare leaders’ needs to better serve their organizational missions as care providers and employers in their communities.
The expert panelists included Zach Goodling, Director, Population Health and Care Coordination at Multicare; Randy Osteen, VP Applications, Information Management at CHRISTUS Health; and Ruth Krystopolski, SVP of Population Health at Atrium Health.
The panel discussion gave attendees the opportunity to:
- Understand experiences and lessons learned from industry population health and informatics leaders in preparing for value-based care opportunities to improve care quality and reduce costs in their communities
- Learn about approaches to data aggregation and analytics to support population health’s strategic and operational priorities
- Gain an understanding of various care models deployed by different organizations to manage high risk populations
- Appreciate the organizational culture and leadership challenges faced within each of the value-based care journeys of three different dynamic organizations
The discussion began by recognizing that the current state of healthcare is isolated and disconnected; it has interoperability challenges, misaligned incentives for employers, payers, providers, and community services; it tends to focus on sickness for an uninformed and confused user population; and it places accountability on providers that often results in duplication or even scarcity of services.
The opportunity here is tremendous! We can find ways to:

- Enhance the ability to improve care quality and consumer (patient, member, employee) quality of life and reduce the cost of care.
- Come together in consumer-centric manner, using interoperable, technology-enabled, data-driven, innovative business models that cross stakeholder boundaries and focus on quality of life across the continuum of care and services, acknowledging shared risk and creating a more accountable consumer population.
Key messages from the group were enlightening and reflected the progression of the entire healthcare industry.
We heard from all three panelists about the arduous work required to make even small amounts of progress. “We have been on a five-year journey to create capabilities in population health management, managing plans to assist members, identify care gaps, and develop care plans.” The topic of data arose throughout our interviews. The panel discussed various concerns around data aggregation. “The biggest hurdle is aggregating data from non-affiliated places and various systems.” “Data is vital to supporting a broad view of each patient; without it, it is very difficult.” And they cautioned organizations about relying on too much data. “When it comes to analytics, being more actionable is better than gathering more data.”
Many leaders find the array of solutions and systems available to healthcare organizations overwhelming. Our experts provided some insight on platform strategy. “Must identify consistent, reliable, scalable solutions. It is difficult when you have too many solutions/platforms. If you can get users onto the same system, even if it is not the best of class, using the same governance model and tools creates important consistency and scale.”
The panelists had some ideas about other success factors beyond the tool set. “Social determinants are often the biggest impact when managing a population. We joke that we are all social workers. We are putting these resources in place and able to monitor 400-450 patients with some of the highest risk patient populations.” They encouraged a paradigm shift for those setting strategy for value based care. “I am often impressed by the level of expertise in healthcare, but surprised by the lack of awareness about the macro environment. We need to ensure we help our people understand the “why” behind the need for change. The organizational work pales in comparison to the cultural changes required to make progress.” Several panelists also reinforced the long-term focus required for value based care programs to succeed. “This is an iterative process that will evolve over time, not a program with a beginning and end.”
Key Themes from Panelists
- A clearly defined leadership strategy and commitment are imperative.
- Most organizations are still in the early stages of defining their value based care processes. They are working to improve their understanding of consumer engagement and activities that potentially influence consumers. They are exploring new ways of leveraging technologies to engage consumers and provide new models of care.
- The lack of interoperability makes data aggregation difficult and the application of meaningful analytics even more challenging.
A Value Based Care Model
Understanding these key themes provides healthcare leaders with a better understanding of where to focus their efforts, but they still need a model to navigate the various domains of value based care. The model below includes five areas of consideration for healthcare leaders to use as they continue to define their value based care efforts.
- Leadership Strategy & Commitment: Define, refine, and commit to a strategy that allows the organization to realize the benefits of value based care. Leadership engagement is imperative and has the power to accelerate or limit the amount of progress in every domain.
- Data Aggregation: Compilation of disparate clinical, financial, social, supply chain, administrative, public, and consumer data is vital for supporting clinical and business decisions.
- Data Analytics and Business Intelligence: The ability to utilize aggregated data to make informed clinical and business decisions that improve quality, reduce costs, and offer value to consumers
- Models of Care: Leveraging digital technology as appropriate, selection of a care delivery model based on collaboration and communication among all health care providers, payers, consumers, and community resources that contribute to individual consumers’ health and well-being
- Consumer Engagement: Connection and engagement between external stakeholders (consumers) and organizations (company or brand) through various channels of correspondence. This connection can be a reaction, interaction, effect, or overall customer experience that takes place online and offline.

Maturity and Organizational Evaluation
An example of the progression in organizational competency within each dimension is shown below, focusing on the most important dimension: Leadership Strategy and Commitment.

Value based care domains establish a critical foundation for assessing progress. Organizations can then begin to evaluate their maturity within each domain. Atos is developing an innovative algorithm to rank organizational maturity within each domain, as seen in the following chart:
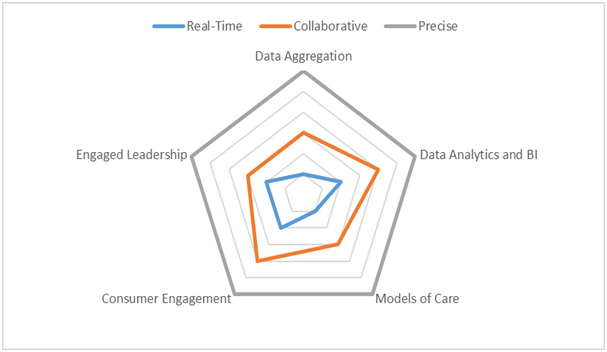
This type of insight helps healthcare leaders to think more strategically about where they invest and how they prioritize the many competing initiatives that impact value based care. This strategic view often results in new operating models and elucidates new ideas, innovative approaches, and ultimately better outcomes for consumers, both inside and outside of the healthcare system.
Atos believes that the digital transformation in healthcare is facing three shockwaves:
- Shockwave 1: Requires leaders to rationalize and streamline existing systems, notably through real-time clinical delivery and an EHR, in addition to the integration of financial, revenue cycle, and clinical data to fully understand care quality and costs that impact overall revenue and the organization’s financial viability
- Shockwave 2: Interconnect and increase collaboration between all ecosystem players, notably through collaboration and digital solutions. Deeply analyze and optimize treatments with new big data and cognitive technologies for population health (achieve early detection of epidemics, discover new risk factors, uncover new treatments, etc.). This is also at the heart of the research in which Atos is participating.
- Shockwave 3: Leverage the latest advances in artificial intelligence, machine learning, and genomics analysis. Leverage high performance computing solutions to enable precision medicine. This is probably the most striking advance on the healthcare horizon.

It will be no small feat for organizations to navigate these shockwaves, respond to ongoing payment reform, and address a changing consumer population; it will require discipline and focus. A complete, thoughtful approach will enable healthcare organizations to move from systems of reactive, disconnected care to a global health system that supports individuals throughout their lives.
About the Authors:
- Mary Sirois is the Vice President of Integrated Solutions Delivery, focused on population health and value-based care services and technology delivery across all of Atos’ solutions. In addition, Ms. Sirois is a member of the Atos Scientific Community.
- Heather Haugen is the Chief Science Officer for Digital Health Solutions for Atos.
- Inbal Vuletich serves as the editor for Atos Digital Health Solution publications.
About Atos Digital Health Solutions
Atos Digital Health Solutions helps healthcare organizations clarify business objectives while pursuing safer, more effective healthcare that manages costs and engagement across the care continuum. Our leadership team, consultants, and certified project and program managers bring years of practical and operational hospital experience to each engagement. Together, we’ll work closely with you to deliver meaningful outcomes that support your organization’s goals. Our team works shoulder-to-shoulder with your staff, sharing what we know openly. The knowledge transfer throughout the process improves skills and expertise among your team as well as ours. We support a full spectrum of products and services across the healthcare enterprise including Population Health, Value-Based Care, Security and Enterprise Business Strategy Advisory Services, Revenue Cycle Expertise, Adoption and Simulation Programs, ERP and Workforce Management, Go-Live Solutions, EHR Application Expertise, as well as Legacy and Technical Expertise. Atos is a proud sponsor of Healthcare Scene.














It won’t just require discipline and focus – it will require huge investments of money and human resources. Implementing a data integration hub in our EHR will cost thousands of dollars, and that’s just so we can exchange data from members of an HIE that we’ll need to join, which will cost thousands annually. And that’s just “Shockwave 2” – I can only imagine the cost of artificial intelligence, machine learning, and genomics analysis.
Karen,
There will be costs, but will the savings outweight the costs? That’s the more challenging question. Costs are fine as long as they’re counterbalanced by savings.
True, John. But only those who can afford the investment will be able to get in the game initially. I guess that’s always the way.
Funny, I just saw this in my LinkedIn feed. Cincinnati Children’s already investing in AI. https://www.linkedin.com/feed/update/urn:li:activity:6466636922553987072/
Everyone will have elements of AI this year. It’s just to what extent. What’s interesting with AI is that it’s most likely to come from vendors that will be happy to sell it to any organization. So, there’s a chance it could be made available to many organizations and not just the richest, but we’ll see.