The headlines are stark and accusatory. “ACOs’ health IT capabilities remain rudimentary.” “ACOs held back by poor interoperability.” But a recent 19-page survey released by the eHealth Initiative tells two stories about Accountable Care Organizations–and I find the story about interoperability less compelling than another one that focuses on patient empowerment.
Certainly, ACOs’ hunger for data is axiomatic. They need to share huge amounts of data internally both to maximize their own resource usage and to treat the whole patient. They need health information exchange (HIE) with outside institutions so they can incorporate insights from them when patients choose to go outside for care. They need population health measures, clinical decision support, and more.
An example of data deprivation can be found in a Government Accountability Office report that tried to figure out why most of the health providers hand-picked by CMS to demonstrate the benefits of accountable care failed to achieve the measly 2% cost improvement set as their goal–even though they produced sterling results on most measurements of improved health care.
The GAO concluded that the problem was lack of data–specifically, feedback on the results of their efforts. CMS possessed the claims data that could be used to generate that feedback, but the data was not exploited. On the CMS side, they took up to two years to crunch the numbers in order to produce actionable feedback. On the provider side, they lacked the tools to do the analysis themselves.
The trade press has routinely released similarly dismal stories about failures to produce high-quality data, to exchange it, and to run analytics. The ACOs were thrown into a data-poor environment characterized by electronic health records loaded with low-quality data (often in unstructured text) and immature standards for health information exchange.
Amazing, then, that a number of advances were reported by the eHealth Initiative report. But the failures dominate. Most notably, “patient safety, cost containment, efficiency, and patient satisfaction” did not improve among the majority of ACOs (p. 15).
This was the other major finding of the eHealth Initiative survey, and one I saw no headlines about. Perhaps the health IT field likes to obsess over data, but I expect that clinicians would give up a lot of population health statistics and other numbers for a closer relationship with the patient. Yet ACOs are not taking advantage of opportunities to involve patients in their own health.
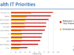
The range of modern tools for empowerment is wide. A shame they are so narrowly deployed. “Few ACOs to date report patient-facing tools that could increase access to care, such as self-service scheduling (33%), phone-based telemedicine (28%) or video-based telemedicine (24%). ACOs are even less likely to offer patients self-management tools such as remote monitoring devices (26%), untethered personal health record (17%), or smartphone apps (15%). (p. 11)
A video connection with a clinician or an app to encourage exercise will probably produce health improvement faster than analytics–although I am a firm believer in analytics as well. Given that ACOs are having trouble finding good tools for data, why don’t they start by turning to everyday tools such as smartphones and using these things to strengthen their impact on patients?
There are risks in patient empowerment as well. The efficacy of most apps has not been proven. Engagement with patients requires more staff time, and this means hiring staff with the right training (and salaries lower than an MD gets).
Patient empowerment and data also intersect, mostly in the area of patient-generated data. But it doesn’t hurt for ACOs to take it slowly, using low-tech means to pick low-hanging fruit and make health a 24/7 concern for the people under their charge. At the same time, they can work over a longer term to add data collection and analysis to their toolbox.













The obvious answer is patients should always come first. Unfortunately focusing on individual patient need was not part of Obamacare and all of the bureaucracy that has been created from it.
ACO’s are the government’s version of HMO’s. What is the definition of insanity doing the same thing over ….. and expecting different results.??
The enormous amount of money that has been diverted to HIT has taken resources away from patient care. Yes, the use of information makes sense and it should be implemented. Unfortunately not meeting the patient needs first (improving health outcomes) results in the adoption of unproven technology including EMR systems that haven’t demonstrated the ability to meet this patient need.
Re: Accountable Care
Patient first, data needed for decion-making at the patient level, other data, in that order.
Aside from all of the mandated data collection, internal healthcare facility need for data and information needed to make bedside decisions, we should never lose focus on the fact that the patient wants out as soon as practicable, with the proviso of no near-term relapse/return.
Does this not tell us that the Case level focus from the time the pt presents should be on discharge planning? (pt gets to go home, beds become available, providers are able to focus on other pts).
The problem of course is that each pt is unique in terms of when they can/should be discharged.
So, we clearly need at the Case level a non-subjective in-your-face means of tracking progress toward pre-defined discharge objectives (this pt can be discharged because they are in a residence with a 24 x 7 nurse foe emergency contact purposes, this pt can go home because they have access to a visiting nurse, this one because they have a caregiver, NOT this one because they live alone and have no support system)
When setting up a set of discharge objectives, some related, some not, it is NOT always essential that all get met, or that all of a short list of pre-defined objectives get met.
The right approach is Cases get closed when Case Managers close them, not when some algorithm posts a discharge advisory.
The Rand Corporation figured out how to manage conflicting needs back in the 1960s.
Adapting this from their application area (missile range, accuracy, payload) to healthcare discharge planning required a bit of out-of-the-box thinking but my group now promotes FOMM (Figure of Merit Matrix) as a default form (spreadsheet actually) at patient Cases.
I have a feeling, Karl, that no patient is psychologically prepared for discharge, and that all will need follow-up afterward. Your intensive approach to planning looks interesting.
And Robert, it’s well worth checking out this posting on patient engagement, which makes it something of an end in itself–or at least an easier thing to focus on than outcomes:
http://thehealthcareblog.com/blog/2014/11/10/pay-for-engagement-a-new-framework-for-physician-reimbursement